Vitamins, Fat-Soluble
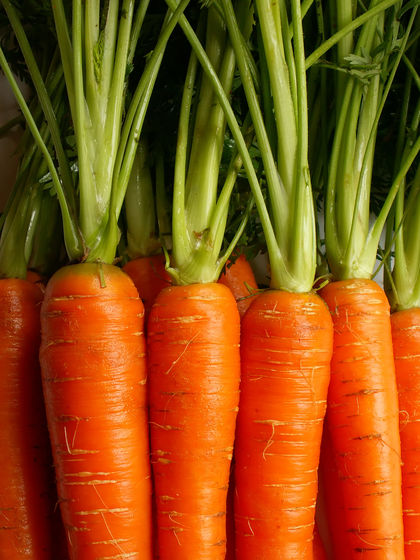
Because they dissolve in fat , vitamins A, D, E, and K are called fat-soluble vitamins. They are absorbed from the small intestines , along with dietary fat, which is why fat malabsorption resulting from various diseases (e.g., cystic fibrosis, ulcerative colitis, Crohn's disease) is associated with poor absorption of these vitamins. Fat-soluble vitamins are primarily stored in the liver and adipose tissues . With the exception of vitamin K, fat-soluble vitamins are generally excreted more slowly than water-soluble vitamins, and vitamins A and D can accumulate and cause toxic effects in the body.
Vitamin A
Vitamin A was the first fat-soluble vitamin identified (in 1913). Vitamin A comprises the preformed retinoids, plus the precursor forms, the provitamin A carotenoids . Preformed retinoids is a collective term for retinol, retinal, and retinoic acid, all of which are biologically active. The provitamin A carotenoids include beta-carotene and others, which are converted to retinoids with varying degrees of efficiency. Retinoids are sensitive to heat, light, and oxidation by air. Beta-carotene is relatively more stable. Vitamin E helps protect vitamin A from oxidation. There is some loss of vitamin A with cooking, but only after boiling for a comparatively long period.
Retinoids are converted to retinol in the intestines and transported with dietary fat to the liver, where it is stored. A special transport protein , retinolbinding protein (RBP), transports vitamin A from the liver to other tissues. Carotenoids are absorbed intact at a much lower absorption rate than retinol. Of all the carotenoids, beta-carotene has the highest potential vitamin-A activity. The active forms of vitamin A have three basic functions: vision, growth and development of tissues, and immunity.
- Vision. Vitamin A combines with a protein called opsin to form rhodopsin in the rod cells of the retina. When vitamin A is inadequate, the lack of rhodopsin makes it difficult to see in dim light.
- Growth and development of tissues. Vitamin A is involved in normal cell differentiation—a process through which embryonic cells transform into mature tissue cells with highly specific functions. Vitamin A supports male and female reproductive processes and bone growth.
- Immunity. Vitamin A is essential for immune function and vitamin-A deficiency is associated with decreased resistance to infections. The severity of some infections, such as measles and diarrhea, is reduced by vitamin-A supplementation among those who suffer from vitamin-A deficiency.
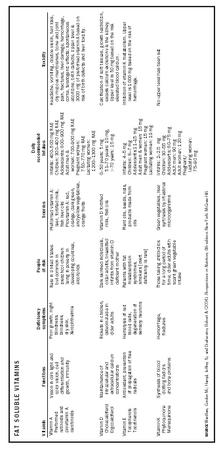
| Vitamin | Functions | Deficiency symptoms | People at risk | Sources | Daily recommended intakes | Toxicity |
| SOURCE Wardlaw, Gordon M.; Hampl, Jeffrey S.; and Disilvestro, Robert A. (2004). Perspectives in Nutrition , 6th edition. New York: McGraw-Hill. | ||||||
| Vitamin A Preformed retinoids and provitamin A carotinoids | Vision in dim light and color vision, cell differentiation and growth, immunity | Poor growth, night blindness, blindness, dry skin, Xerophthalmia | Rare in United States but common in preschool children living in poverty in developing countries, alcoholics | Preformed vitamin A: liver, fortified milk, fish liver oils Provitamin A: red, orange, dark green, and yellow vegetables, orange fruits | Infants: 400-500 mg RAE Children: 300-400 mg RAE Adolescents: 600-900 mg RAE Adult men & women: 700-900 mg RAE Pregnant women: 750-770 mg RAE Lactating women:1200-1300 mg RAE | Headache, vomiting, double vision, hair loss, dry mucous membranes, bone and joint pain, fractures, liver damage, hemorrhage, coma, teratogenic effects: spontaneous abortions, birth defects. Upper level is 3000 mg of preformed vitamin A based on risk of birth defects and liver toxicity. |
| Vitamin D Cholecalciferol Ergocalciferol | Maintainence of intracellular and extracellular calcium concentrations | Rickets in children, osteomalacia in older adults | Dark skinned individuals, older adults, breastfed infants from vitamin D deficient mother | Vitamin D fortified milk, fish oils | 0-50 years: 5 mg 51-70 years: 10 mg, >70 years: 15 mg | Calcification of soft tissues, growth restriction, excess calcium excretion via the kidney. Upper level is 50 mg based on the risk elevated blood calcium. |
| Vitamin E Tocopherols Tocotrienols | Antioxidant, prevention of propagation of free radicals | Hemolysis of red blood cells, degeneration of sensory neurons | Patients with fat malabsorption syndromes, smokers [overt deficiency is rare] | Plant oils, seeds, nuts, products made from oils | Infants: 4-5 mg Children: 6-7 mg Adolescents:11-15 mg Adult men & women: 15 mg Pregnant women: 15 mg Lactating women: 19 mg | Inhibition of vitamin K metabolism. Upper level is 1000 mg based on the risk of hemorrhage. |
| Vitamin K Phylloquinone Menaquinone | Synthesis of blood clotting factors and bone proteins | Hemorrhage, fractures | Those taking antibiotics for a long period of time; older adults with scant green vegetable intake | Green vegetables, liver synthesis by intestinal microorganisms | Infants: 2-2.5 mg Children: 30-55 mg Adolescents: 60-75 mg Adult men: 90 mg Adult women: 120 mg Pregnant/lactating women: 75-90 mg | No upper level has been set |
It has been suggested that beta-carotene and other carotenoids (also called phytochemicals ) may function as antioxidants by neutralizing free radicals . Free radicals are unstable, highly reactive molecules that damage DNA , cause cell injury, and increase the risk of chronic disease. Beta-carotene has also been associated with reducing the risk of lung cancer . Lutein and zeaxanthin, yellow carotenoid pigments in corn and dark green leafy vegetables, may reduce the risk of macular degeneration and agerelated cataracts . Lycopene, a red carotenoid pigment in tomatoes, may help reduce the risk of prostrate cancer, cardiovascular disease, and skin damage from sunlight.
Deficiency.
Dietary deficiency of vitamin A is rare in North America and western Europe, but it is the leading cause of blindness in children worldwide. Newborn and premature infants, the urban poor, older adults, people with alcoholism or liver disease, and those with fat malabsorption syndrome are all at increased risk.
One of the earliest symptoms of vitamin-A deficiency is night blindness. It is a temporary condition, but if left untreated it can cause permanent blindness. This degeneration is called xerophthalmia, and it usually occurs in children after they are weaned. Symptoms include dryness of the cornea and eye membranes due to lack of mucus production, which leaves the eye vulnerable to surface dirt and bacterial infections. Vitamin-A deficiency can cause follicular hyperkeratosis, a condition in which hair follicles become plugged with keratin, giving a bumpy appearance and a rough, dry texture to skin.
In developing countries, the severity of infectious diseases such as measles is often correlated to the degree of vitamin-A deficiency. Providing large doses of vitamin A reduces the risk of dying from these infections. The age range of the target population for vitamin-A intervention programs is usually from birth to seven years. Administration of high-potency doses in the range of 15,000 to 60,000 micrograms (μg) are distributed to young children in targeted areas of the world to build up liver stores for up to six months. However, consumption of adequate food sources is the most important long-term solution to vitamin-A deficiency.
Toxicity.
Vitamin-A toxicity, called hypervitaminosis A, can result from long-term supplementation of two to four times the RDA for preformed vitamin A. Excess intake of preformed vitamin A is a teratogen, meaning it can cause birth defects. Birth defects associated with vitamin-A toxicity include cleft palate, heart abnormalities, and brain malfunction. Acute excess intake during pregnancy can also cause spontaneous abortions. Pregnant women should avoid prenatal supplements containing retinal, as well as medications made from retinoids, such as Accutane and Retin-A. Prolonged and excessive consumption of carotene-rich foods can lead to hypercarotenemia, a clinical condition characterized by deep orange discoloration of the skin and increased carotene levels in the blood. This condition is usually harmless.
Vitamin D (Calciferol)
In the seventeenth century, vitamin-D deficiency was so common in British children that it came to be known as "children's disease of the English." In
![Sunlight stimulates the synthesis of vitamin D, which regulates the body's absorption of calcium and therefore is essential to skeletal health. Just fifteen minutes in the sun several times weekly is sufficient. After that, sunscreen should be applied to avoid ultraviolet damage to the skin. [Photograph by Michael Keller. Corbis. Reproduced by permission.]](../images/nwaz_02_img0230.jpg)
Vitamin D from foods is absorbed from the upper part of the small intestine, along with dietary fat, and transported to the liver. In the skin, ultraviolet (UV) radiation from the sun converts a cholesterol derivative to cholecalciferol, which enters the blood stream and is transported to the liver. In the liver, vitamin D is converted to calcidiol, an inactive form that circulates in blood. Kidneys take up calcidiol and convert it to an active hormone form of vitamin D called calcitriol. People with chronic kidney failure have very low levels of calcitriol and must be routinely treated with this form of the vitamin.
The best-known function of active vitamin D is to help regulate blood levels of calcium and phosphorous. Vitamin D increases absorption of these minerals from the gastrointestinal (GI) tract. In combination with parathyroid hormone, it enhances their reabsorption from the kidneys and their mobilization from bones into the blood. Vitamin D helps maintain calcium levels even if dietary intakes are not optimal. Calcitriol affects growth of normal cells and some cancer cells. Adequate vitamin-D status has been linked to a reduced risk of developing breast, colon, and prostrate cancers.
Deficiency.
Long-term deficiency of vitamin D affects the skeletal system. In children, vitamin-D deficiency leads to rickets, a condition in which bones weaken and bow under pressure. Although vitamin-D fortification has reduced incidence of rickets in North America, it is sometimes seen in children with malabsorption syndrome and is still common in many parts of the world. In adults, vitamin-D deficiency causes osteomalacia , or "soft bones," increasing the risk for fractures in hip, spine, and other bones. Vitamin-D deficiency also contributes to osteoporosis . In elderly persons, vitamin-D supplementation reduces the risk of osteoporotic fractures.
Infants are born with stores of vitamin D that last about six months. Breast milk contains very little vitamin D, however, and infants beyond six months of age who are exclusively breastfed must obtain vitamin D via exposure to sunlight or a supplement given under the guidance of a physician.
Older adults are especially at risk for vitamin-D deficiency for several reasons. The skin, liver, and kidneys lose their capacity to synthesize and activate vitamin D with advancing age, and older adults typically drink little or no milk, a major dietary source of vitamin D. Older adults also rarely venture outdoors, and when they do, they apply sunscreen to exposed areas of the body, further contributing to the decline in vitamin-D synthesis in the skin.
Sunscreens with a sun protection factor (SPF) of 8 and above prevent vitamin-D synthesis. Sunscreen should be applied only after enough time has elapsed to provide sufficient vitamin-D synthesis. Exposure to the sun does not cause vitamin-D toxicity, and for most people, exposing the hands, face, and arms on a clear summer day for fifteen minutes a few times a week should provide sufficient Vitamin D. Dark-skinned people require longer sunlight exposure because melanin, a skin pigment, is a natural sunscreen.
Dietary recommendations assume that no vitamin D is available from exposure to sunlight. Thus, people who do not venture outdoors or who live in northern or predominantly cloudy climates need to pay attention to dietary sources. Plants are poor sources of vitamin D, so strict vegetarians must meet their vitamin-D needs through exposure to sunlight, fortification, or supplementation.
Toxicity.
Vitamin D is most likely to have toxic effects when consumed in excessive amounts through supplementation. Excess vitamin D raises blood calcium levels, resulting in calcium precipitation in soft tissues and stone formation in the kidneys, where calcium becomes concentrated in an effort to excrete it.
Vitamin K
In 1929, the Danish researcher Henrik Dam first noted that vitamin K played a critical role in blood clotting , and he named it vitamin "K" for "Koagulation." Vitamin K comprises a family of compounds known as quinones. These include phylloquinone from plants and the menaquinones from animal sources. Phylloquinone is the most biologically active form. Menaquinones are also synthesized by bacteria in the colon and absorbed, contributing about 10 percent of total vitamin-K needs. Vitamin-K absorption depends on normal consumption and digestion of dietary fat. It is primarily stored in the liver.
Vitamin K helps in the activation of seven blood-clotting-factor proteins that participate in a series of reactions to form a clot that eventually stops the flow of blood. Vitamin K also participates in the activation of bone proteins, which greatly enhances their calcium-binding properties. Low levels of circulating vitamin K have been associated with low bone-mineral density. Thus, an adequate intake of vitamin K may help protect against hip fractures.
Deficiency.
A primary deficiency of vitamin K is rare, but a secondary deficiency may result from fat malabsorption syndrome. Prolonged use of antibiotics can destroy the intestinal bacteria that produce vitamin K, precipitating deficiency in individuals at risk. Newborn infants are born with a sterile intestinal tract and those who are breastfed, may run the risk of vitamin-K deficiency, since breast-milk production takes a few days to establish and breast milk is naturally low in this vitamin. To prevent hemorrhaging, all infants in North America receive injections of vitamin K within six hours of birth.
Toxicity.
High doses of vitamin K can reduce the effectiveness of anticoagulant drugs such as warfarin (Coumadin), which is used to prevent blood clotting. People taking these drugs should maintain a consistent daily intake of vitamin K. Megadose supplements of vitamin A and E can pose a risk to vitamin-K status. Vitamin A interferes with absorption of vitamin K, and large doses of vitamin E decrease vitamin K–dependent clotting factors, thus promoting bleeding. Toxicity from food is rare, because the body excretes vitamin K much more rapidly than other fat-soluble vitamins.
Vitamin E
The link between vitamin-E deficiency and reproductive failure in rats was first discovered in 1922 by Herbert Evans and Katherine Scott Bishop. The chemical name of vitamin E, tocopherol, is derived from toco, meaning "related to childbirth."
Vitamin E comprises a family of eight naturally occurring compounds: four tocopherols and four tocotrienols, of which alpha-tocopherol is the only one to have vitamin-E activity in the human body. It is also the most common form of vitamin E in food. Vitamin E is highly susceptible to destruction by oxygen , metals, light, and deep-fat frying. As a result, prolonged food storage lowers the vitamin-E content of food.
As with other fat-soluble vitamins, absorption of vitamin E requires adequate absorption of dietary fat. In addition, the percentage of absorption declines as the amount consumed is increased. Vitamin E is stored mainly in adipose tissue, while some is stored in the muscle. The remaining vitamin E is found in cell membranes in tissue.
Vitamin E is an antioxidant and one of the body's primary defenders against oxidative damage caused by free radicals. Its activity is enhanced by other antioxidants such as vitamin C and the mineral selenium. Vitamin E interrupts free-radical chain reactions by getting oxidized, thus protecting cell membranes from free-radical attack. Scientists have implicated oxidative stress in the development of cancer, arthritis , cataracts, heart disease , and in the process of aging itself. However, it is not yet known whether supplementation with megadoses of vitamin E offers protection against heart disease and cancer beyond that provided by positive dietary and lifestyle changes.
Deficiency.
Due to the widespread use of vegetable oils, primary vitamin-E deficiency is rare. Most deficiencies occur in people with fat malabsorption syndrome. Smokers and adults on very low-fat diets are at increased risk of developing vitamin-E deficiency. Preterm infants are particularly susceptible to hemolytic anemia (anemia caused by the destruction of red blood cells) due to vitamin-E deficiency. These infants are born with limited stores of vitamin E, which are exhausted by rapid growth, and they are inefficient in absorbing vitamin E from the intestinal tract. Without vitamin E to protect against oxidation, the destruction of cell membranes causes red blood cells to burst. To prevent hemolytic anemia, special formulas and supplements containing vitamin E are prescribed for preterm infants.
Toxicity.
Large doses of vitamin E can counter the actions of vitamin K and decrease the production of vitamin K–dependent clotting factors, thus promoting serious hemorrhaging effects in adults. Individuals who are vitamin-K deficient or who are taking anticoagulant medications such as warfarin or aspirin are especially at risk from megadoses of vitamin E.
SEE ALSO Vitamins, Water-Soluble .
Kiran B. Misra
Bibliography
Insel, Paul; Turner, Elaine R.; and Ross, Don (2002). Nutrition. Sudbury, MA: Jones and Bartlett.
Wardlaw, Gordon M.; Hampl, Jeffrey S.; and Disilvestro, Robert A. (2004). Perspectives in Nutrition, 6th edition. New York: McGraw-Hill.
Whitney, Eleanor Noss, and Rolfes, Sharon Rady (2002). Understanding Nutrition, 9th edition. Belmont, CA: Wadsworth/Thomson Learning.

Comment about this article, ask questions, or add new information about this topic: