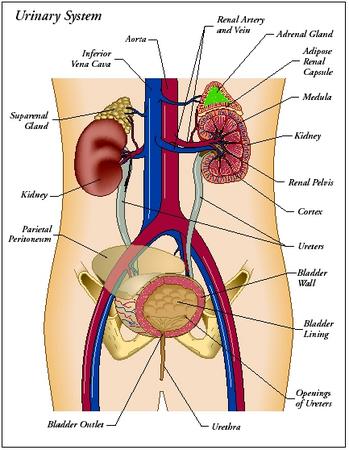
The Urinary System - Design: parts of the urinary system
The main organs of the urinary system are the kidneys, which form urine. The other parts of the system—the ureters, the urinary bladder, and the urethra—neither form urine nor change its composition. They are merely structures that transport urine from the kidneys to the outside of the body.
The kidneys
The kidneys are kidney bean-shaped organs located on either side of the vertebral column or spine near the small of the back (the beans were so named because they resembled small kidneys). The left kidney usually sits slightly higher than the right one. The size of an adult kidney is approximately 4 inches (10 centimeters) long, 2.5 inches (6 centimeters) wide, and 1 inch (2.5 centimeters) thick. The upper portions of the purplish-brown kidneys rest on the lower surface of the diaphragm, a membrane of muscle separating the thoracic or chest cavity from the abdominal cavity. The lower portion of the rib cage encloses and protects the kidneys. The kidneys are held in place by the abdominal lining and supporting connective tissue.
On the side of each kidney facing the vertebral column is an indentation called the hilus. Through the hilus the renal artery enters and the renal vein and ureter exit (the adjective renal comes from the Latin word renes , meaning "kidneys"). The renal artery brings blood to the kidneys from the abdominal
- Aldosterone (al-DOS-te-rone):
- Hormone secreted by the adrenal cortex that controls the salt and water balance in the body.
- Antidiuretic hormone (an-tee-die-yu-REH-tik HOR-mone):
- Hormone produced by the hypothalamus and stored in the posterior pituitary that increases the absorption of water by the kidneys.
- Bowman's capsule (BOW-manz KAP-sul):
- Cupshaped end of a nephron that encloses a glomerulus.
- Calyces (KAY-li-seez):
- Cup-shaped extensions of the renal pelvis that enclose the tips of the renal pyramids and collect urine.
- Creatinine (kree-AT-i-neen):
- Waste product in urine produced by the breakdown of creatine.
- Filtration (fill-TRAY-shun):
- Movement of water and dissolved materials through a membrane from an area of higher pressure to an area of lower pressure.
- Glomerulus (glow-MER-yoo-lus):
- Network of capillaries enclosed by a Bowman's capsule.
- Henle's loop (HEN-leez LOOP):
- Looped portion of a renal tubule.
- Hilus (HIGH-lus):
- Indentation or depression on the surface of an organ such as a kidney.
- Micturition (mik-tu-RISH-un):
- Urination, or the elimination or voiding of urine from the urinary bladder.
- Nephrons (NEFF-ronz):
- Urine-forming structures in the kidneys.
- Peristalsis (per-i-STALL-sis):
- Series of wavelike muscular contractions that move material in one direction through a hollow organ.
- Renal corpuscle (REE-nul KOR-pus-el):
- Part of a nephron that consists of a glomerulus enclosed by a Bowman's capsule.
- Renal cortex (REE-nul KOR-tex):
- Outermost layer of the kidney.
- Renal medulla (REE-nul muh-DUH-luh):
- Middle layer of a kidney.
- Renal filtrate (REE-nul FILL-trait):
- Fluid formed in a Bowman's capsule from blood plasma by the process of filtration in the renal corpuscle.
- Renal pelvis (REE-nul PELL-vis):
- A cavity at the innermost area of a kidney that connects to the ureter.
- Renal pyramids (REE-nul PEER-ah-mids):
- Triangular or pie-shaped segments of the renal medulla in which urine production occurs.
- Renal tubule (REE-nal TOO-byool):
- Twisting, narrow tube leading from the Bowman's capsule in a nephron.
- Renin (REE-nin):
- Enzyme secreted by the cells of renal tubules that helps to raise blood pressure.
- Urea (yoo-REE-ah):
- Main nitrogen-containing waste excreted in the urine, produced when the liver combines ammonia and carbon dioxide.
- Ureter (you-REE-ter):
- Muscular tube that carries urine from the renal pelvis in a kidney to the urinary bladder.
- Urethra (yoo-REE-thrah):
- Thin-walled tube that carries urine from the urinary bladder to the out-side of the body.
- Uric acid (YUR-ik AS-id):
- Waste product in urine formed by the breakdown of nucleic acids.
- Urinary bladder
- (YER-i-nair-ee BLA-der) Hollow, collapsible, muscular sac that stores urine temporarily.
- Urine (YUR-in):
- Fluid formed by the kidneys from blood plasma.
aorta. The renal vein returns blood to the inferior vena cava. Both the renal artery and renal vein have a right and left branch, each connected to a corresponding kidney.
Each kidney is covered with a thin yet tough capsule of fibrous connective tissue. The transparent capsule gives a kidney a glistening appearance. Inside, a kidney can be divided into three layers. The outer layer, light in color, is called the renal cortex. The next layer, a darker reddish-brown, is called the renal medulla. It contains six to eighteen pie-shaped structures called renal pyramids, the tips of which face toward the center of a kidney.
Attached to the tips of the renal pyramids are cup-shaped tubes called calyces (singular: calyx), which collect urine from structures in the renal pyramids. The smaller calyces unite to form larger calyces, which in turn unite to form the renal pelvis, a cavity at the innermost part of a kidney. The renal pelvis collects urine from the calyces and funnels it to the ureter, to which it is attached.
NEPHRONS. The urine-forming structures in the kidneys are called nephrons. There are approximately 1.25 million nephrons in each kidney. Almost 0.5 inch (1.2 centimeters) in length, each nephron begins in the lower portion of the renal cortex, then twists and coils down into a renal pyramid in the renal medulla. A nephron has two major portions: a renal corpuscle and a renal tubule.
The renal corpuscle is a knotted network of fine capillaries surrounded by a cup-shaped chamber. The knot of capillaries is called a glomerulus (plural: glomeruli). The cup-shaped chamber is called the Bowman's capsule, and it is filled with fluid and has an inner and outer wall. The inner wall encloses the glomerulus and has many pores that make it permeable or able to allow fluids or material to pass easily through it. Its outer wall has no pores and is, thus, not permeable.
It is not necessary for an individual to have two kidneys in order to live. In fact, one kidney can easily perform the job of two, filtering wastes from the body and creating urine. People who have only one kidney because of an illness or because they donated a kidney for transplantation can and do lead healthy lives. When only one kidney is functioning in the body, it usually increases in size by 50 percent in order to perform well.
The renal tubule is a long passageway that continues from the Bowman's capsule. It twists and turns down through a renal pyramid before forming a loop (called Henle's loop) and ascending back through the renal pyramid. As it ascends, it becomes slightly larger. This larger section of the renal tubule twists and coils across the top of the renal pyramid before descending once again. It then empties into a collecting duct that serves several renal tubules. Several collecting ducts then unite to form larger ducts that empty urine into a calyx at the tip of the renal pyramid.
The ureters
The ureters are muscular tubes that carry urine from the renal pelvis in each kidney to the urinary bladder. Each ureter measures about 10 to 12 inches (25 to 30 centimeters) in length, extending from the hilus of a kidney to the rear wall of the urinary bladder, where it enters at an angle. The extremely thin ureters only measure about 0.25 inch (0.64 centimeter) in diameter.
Urine drains through the ureters to the urinary bladder by gravity, but the smooth muscular walls of the ureters also help propel urine along. They compress in a series of wavelike contractions (an action known as peristalsis) that move the urine through the ureters in only one direction. When urine has entered the urinary bladder, it is prevented from flowing back into the ureters by small, valvelike folds of membrane that flap over the ureter openings.
The urinary bladder
The urinary bladder is a hollow, collapsible, muscular sac that stores urine temporarily. It is located in the pelvis behind the pelvic bones, and is held in place by ligaments. In women, the bladder is behind the uterus; in men, it is above the prostate gland.
The size of the urinary bladder varies depending on the amount of urine it contains. When empty, it is normally no longer than 2 to 3 inches (5 to 7.6 centimeters). During this state, its walls are thick and heavily folded. As it begins collecting urine, the urinary bladder's muscular walls stretch and expand, and it rises in the abdominal cavity. A urinary bladder that is moderately full measures about 5 inches (12.7 centimeters) in length and holds just over 1 pint (500 millimeters) of urine. When completely full, the urinary bladder can contain over 2 pints (1 liter) of urine.
The muscular walls of the urinary bladder contract to expel urine out of the bladder into the urethra. A sphincter or ring of muscle surrounding the opening to the urethra, called the internal urethral sphincter, controls the flow of urine. This is an involuntary sphincter, meaning a person cannot consciously control its workings.
The urethra
The urethra is a thin-walled tube that carries urine from the urinary bladder to the outside of the body. Its length and function differ in females and males.
In females, the urethra measures about 1 to 1.5 inches (2.5 to 3.8 centimeters) in length. Its external opening lies in front of the vaginal opening. The only purpose of the urethra in females is to conduct urine to the out-side of the body.
In males, the urethra serves a dual purpose. It transports semen and urine to the body exterior, but never at the same time. Thus, it serves both the reproductive and urinary systems. In men, the urethra extends from the urinary bladder through the prostate gland to the tip of the penis, a distance of 6 to 8 inches (15 to 20 centimeters).
In both sexes, the urethra contains a ring of skeletal muscle that forms the external urethral sphincter as the urethra passes through the floor of the pelvis. A person is normally able to control the opening and closing of this sphincter. When the sphincter is voluntarily relaxed, urine flows into the urethra, emptying the urinary bladder. However, when the bladder fills with urine and becomes stretched beyond normal, voluntary control of the sphincter becomes no longer possible.

Comment about this article, ask questions, or add new information about this topic: