The Reproductive System - Design: parts of the reproductive system
The male and female reproductive systems form the halves that come together to create new human life. Each system is composed of primary and accessory reproductive organs. In both, the primary sex organs are called gonads. These gonads produce reproductive or sex cells called gametes; they also secrete sex hormones. Despite their joint purpose to produce offspring, the two systems are quite different in structure and function.
The male reproductive system
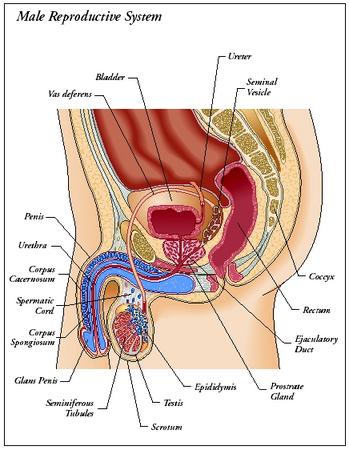
The primary organs in the male reproductive system are the testes. Their main function is to produce male gametes or sperm, which fertilize ova or female eggs (they also produce the male hormone testosterone). The reproductive ducts—epididymis, ductus deferens, ejaculatory duct, and urethra—carry sperm from the testes to the exterior of the body. Accessory glands—seminal vesicles, prostate gland, and bulbourethral glands—produce secretions that combine with sperm to create semen. The male genitalia (external sex organs) are the scrotum and penis.
- Acrosome (AK-ro-sohm):
- Tip of the head of a sperm cell that contains enzymes to digest the membrane of an ovum.
- Adenosine triphosphate (ah-DEN-o-seen try-FOS-fate):
- High-energy molecule found in every cell in the body.
- Amnion (AM-nee-on):
- Fluid-filled sac that surrounds a developing embryo/fetus.
- Areola (ah-REE-oh-lah):
- Circular, darkened area surrounding the nipple of each breast.
- Alveolar glands (al-VEE-o-lar GLANDZ):
- Glands within the lobes of mammary glands that produce milk.
- Bulbourethral glands (bull-bo-yoo-REE-thruhl GLANDZ):
- Glands located underneath on either side of the prostate gland in males that secrete fluid that becomes part of semen.
- Cervix (SIR-viks):
- Lower necklike portion of the uterus leading into the vagina.
- Chromosomes (kro-meh—somes):
- Threadlike structures found in the nucleus of cells that carry the genetic material or genes that determine heredity.
- Circumcision (sirnkum-SIZH-un):
- Surgical removal of the prepuce or foreskin of the penis.
- Clitoris (KLI-to-ris):
- Small protruding mass of erectile tissue at the top of the labia minora.
- Corpus luteum (KOR-pus LOU-tee-um):
- Yellowish remains of a burst ovarian follicle that secretes progesterone.
- Ductus deferens (DUK-tus DEF-e-renz):
- Passageway that carries sperm from the epididymis to the ejaculatory duct.
- Ejaculation (ee-jack-you-LAY-shun):
- Sudden ejection of semen from the penis.
- Ejaculatory duct (ee-JACK-yoo-la-tor-ee DUKT):
- Duct formed by the union of the ductus deferens and the duct of the seminal vesicle.
- Endometrium (en-doe-MEE-tree-um):
- Inner layer of the uterus that provides nourishment for a developing embryo and fetus and that sloughs off during the regular menstrual cycle.
- Epididymis (ep-i-DID-i-mis):
- Portion of the male reproductive duct system in which sperm mature or fully develop.
- Estrogens (ES-tro-jenz):
- Female steroid hormones secreted by the ovaries that bring about the secondary sex characteristics and regulate the female reproductive cycle.
- Fallopian tube (fah-LOH-pee-an TOOB):
- Tube connecting an ovary to the uterus and through which an ovum is transported.
- Fimbriae (FIM-bree-ee):
- Fingerlike projections at the end of a fallopian tube that partially surround an ovary.
- Flagellum (flah-JELL-um):
- Long, whiplike tail that helps provide locomotion in certain cells, such as sperm cells.
- Follicle-stimulating hormone (FAH-lik-uhl STIM-yoolay-ting HOR-mone):
- Gonadotropic hormone produced by the anterior pituitary gland that stimulates the development of follicles in the ovaries of females and sperm in the testes of males.
- Gamete (GAM-eat):
- Female or male reproductive or sex cell (egg or sperm).
- Genitalia (jen-i-TAY-lee-ah):
- External organs of the reproductive system.
- Gonad (GO-nad):
- Sex organ in which reproductive cells develop.
- Greater vestibular glands (GRAY-ter ves-TI-byoo-lar GLANDZ):
- Pair of mucus-secreting glands that lubricate the lower portion of the vagina.
- Hymen (HI-men):
- Thin membrane partially covering the external opening of the vagina.
- Hysterectomy (his-teh-REK-teh-mee):
- Surgical removal of the uterus.
- Labia majora (LAY-bee-ah ma-JOR-ah):
- Outer skin folds of the vagina.
- Labia minora (LAY-bee-ah my-NOR-ah):
- Inner skin folds of the vagina.
- Lactiferous ducts (lak-TIF-er-us):
- Ducts that carry milk from the alveolar glands to the surface of the nipple of a breast.
- Luteinizing hormone (loo-tee-in-EYE-zing):
- Gonadotropic hormone secreted by the anterior pituitary that stimulates, in women, ovulation and the release of estrogens and progesterone by the ovaries and, in men, the secretion of testosterone by the testes.
- Mammary glands (MAM-uh-ree GLANDZ):
- Milk-producing glands in female breasts.
- Menarche (meh-NAR-key):
- Beginning of menstruation or the first menstrual period.
- Menopause (MEN-ah-paws):
- Period in a woman's life when menstrual activity ceases.
- Menstruation (men-stroo-A-shun):
- Also known as menses, periodic (monthly) discharge of blood, secretions, tissue, and mucus from the female uterus in the absence of pregnancy.
- Mons pubis (MONZ PYU-bes):
- Fatty, rounded area at the top of the vulva.
- Myometrium (my-oh-MEE-tree-um):
- Outer layer of the uterus composed of interwoven smooth muscle cells.
- Oocyte (OH-oh-site):
- Immature or developing egg cell.
- Ova (O-va):
- Female gametes or eggs (singular: ovum).
- Ovarian follicles (o-VAR-ee-an FOL-i-kulz):
- Structures within an ovary consisting of a developing egg surrounded by follicle cells.
- Ovaries (O-var-eez):
- Female gonads in which ova (eggs) are produced and that secrete estrogens and progesterone.
- Ovulation (ov-yoo-LAY-shun):
- Release of a mature ovum from an ovary.
- Oxytocin (ahk-si-TOE-sin):
- Hormone produced by the hypothalamus and stored in the posterior pituitary that stimulates contraction of the uterus during childbirth and secretion of milk during nursing.
- Penis (PEE-nis):
- Male organ of reproduction and urination.
- Placenta (plah-SEN-tah):
- Temporary organ that provides nutrients and oxygen to a developing fetus, carries away wastes, and produces hormones such as estrogens and progesterone.
- Prepuce (PREE-pyus):
- Also called foreskin, the fold of skin over the glans or tip of the penis.
- Progesterone (pro-JESS-te-rone):
- Female steroid hormone secreted by the ovaries that makes the uterus more ready to receive a fertilized ovum or egg.
- Prolactin (pro-LAK-tin):
- Gonadotropic hormone secreted by the anterior pituitary that stimulates the mammary glands to produce milk.
- Prostate gland (PRAHS-tate GLAND):
- Muscular gland in males that surrounds the first inch of the urethra and secretes a fluid that becomes part of semen.
- Scrotum (SKROW-tum):
- External sac enclosing the testes.
- Semen (SEE-men):
- Thick, whitish, somewhat sticky fluid composed of sperm and glandular secretions that is propelled out of a male's reproductive tract during ejaculation.
- Seminal vesicles (SEM-i-nuhl VESS-i-kulls):
- Glands in males located at the base of the bladder that secrete fluid that becomes part of semen.
- Seminiferous tubules (sem-i-NIFF-er-us TOO-byoolz):
- Tightly coiled tubes within the testes that produce sperm.
- Sperm:
- Mature male sex or reproductive cell.
- Testes (TESS-teez):
- Male gonads that produce sperm cells and secrete testosterone.
- Testosterone (tess-TAHS-ter-ohn):
- Hormone secreted by the testes that spurs the growth of the male reproductive organs and secondary sex characteristics.
- Umbilical cord (um-BILL-i-kull KORD):
- Structure that connects the embryo/fetus to the placenta.
- Uterus (YOU-ter-us):
- Also known as the womb, the hollow organ in females that receives, retains, and nourishes a fertilized ovum or egg.
- Vagina (vuh-JIGH-nah):
- Muscular tube in women that extends from the cervix of the uterus to the vaginal opening.
- Vulva (VUL-vah):
- Female external genital organs.
- Zygote (ZIE-goat):
- Fertilized ovum.
THE TESTES. The testes are two small, egg-shaped structures suspended in the scrotum, a loose sac of skin that hangs outside the pelvic cavity between the upper thighs. In a male fetus, the testes develop near the kidneys, then descend into the scrotum just before birth.
Each testis measures about 1.5 inches (3.8 centimeters) long and 1 inch (2.5 centimeters) wide. Internally, a testis is subdivided into many lobes. Each lobe contains one to four tightly coiled tubes, called seminiferous tubules, in which sperm is produced. Each tubule averages about 31.5 inches (80 centimeters) in length. The combined length of all the seminiferous tubules in a testis equals about 0.5 mile (0.8 kilometer).
Mature sperm cells are the smallest cells in the body. Each tadpolelike sperm cell consists of three regions: the head, middle piece, and flagellum. The helmetlike head contains the male genetic material essential for reproduction. On the tip of the head is the acrosome, which contains enzymes to break down the membrane of an ovum so fertilization can occur. The middle piece contains a supply of adenosine triphosphate (ATP), a high-energy molecule found in every cell in the body. The sperm cell uses the ATP to power its flagellum, the long whiplike tail, to move the cell along.
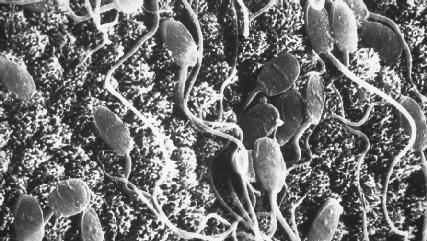
Sperm from the seminiferous tubules are carried along by fluids through a network of tubes before entering the epididymis, the first of the male reproductive ducts.
THE EPIDIDYMIS. The epididymis is a tube about 20 feet (6 meters) in length. Tightly coiled on the posterior or back side of each testis, each epididymis takes up very little room. As sperm cells move through this tube, they absorb nutrients and become mature or fully developed, a process that takes about two weeks. The walls of the epididymis are made of smooth muscle cells, which helps propel sperms cells into the ductus deferens.
THE DUCTUS DEFERENS. The ductus deferens, also called the vas deferens, extends from each epididymis upward over the top of the bladder, then down its back side. The paired ducts measure between 16 and 18 inches (40 and 45 centimeters) in length. Their smooth muscular walls move the sperm along through peristaltic contractions, or a series of wavelike muscular contractions that move material in one direction through a hollow organ.
THE EJACULATORY DUCT. The ejaculatory duct is a short passageway that is formed by the union of a ductus deferens and the duct of a seminal vesicle. Each ejaculatory duct measures just under 1 inch (2.5 centimeters) in length. Both ejaculatory ducts empty sperm (from the ductus deferens) and fluid (from the seminal vesicle) into the single urethra.
THE URETHRA. The urethra extends from the base of the urinary bladder to the tip of the penis, a distance of 6 to 8 inches (15 to 20 centimeters). In males, the urethra serves both the reproductive and urinary systems. It transports sperm (with its fluid) and urine to the body exterior, but never both at the same time. When sperm enters the urethra from the ejaculatory ducts, a sphincter or ring of muscle at the junction of the bladder and urethra closes, keeping urine in the bladder (and also preventing sperm from entering the bladder).
ACCESSORY GLANDS AND SEMEN. The three accessory glands produce secretions that combine with sperm to create a whitish, somewhat sticky mixture called semen. Those secretions (the fluid part of semen) are known collectively as seminal fluid. Ejaculation is the sudden ejection of semen from the penis. A typical ejaculation releases between 0.07 and 0.17 ounce (2 and 5 milliliters) of semen. Although as many as 400 to 600 million sperm are contained in a typical ejaculation, they make up only about 1 percent of the volume of the semen because of their extremely small size.
The seminal vesicles are the first accessory glands to add secretions to sperm. Located at the base of the bladder, their ducts join with the paired ductus deferens to form the ejaculatory ducts. Their thick, yellowish secretion, which makes up about 60 percent of the seminal fluid, contains high amounts of fructose (sugar), vitamin C, and other substances. The secretion helps nourish and activate the sperm as its passes through the reproductive tract.
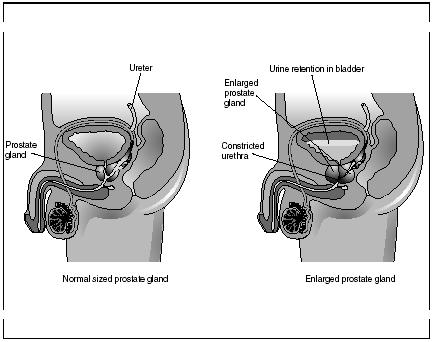
The prostate gland is a single, rounded gland that has a diameter of about 1.6 inches (4 centimeters). It surrounds the urethra as the urethra leaves the bladder. It produces an acidic, milky secretion that enters the urethra through several small ducts. This secretion makes up about 30 percent of the seminal fluid.
The bulbourethral glands are the last glands to add secretions to the seminal fluid. The tiny, pea-shaped glands are located underneath on either side of the prostate gland. Their secretion—a thick, clear mucus—enters the urethra when a man becomes sexually aroused before the secretions of the other accessory glands. The secretion coats the lining of the urethra and cleanses it of any traces of acidic urine that might be present. It also serves as a lubricant during sexual intercourse.
The secretion of all three accessory glands are slightly alkaline or basic (solutions containing a high number of hydrogen ions are acidic, those with a low number are alkaline or basic). This is important because the bacteria present in the female vagina create an acidic environment there. The alkaline seminal fluid neutralizes the acid in the vagina, allowing sperm in the semen to exist and move in the vagina so fertilization may take place.
MALE GENITALIA. The scrotum and penis are the male genitalia that hang outside the body. As stated earlier, the scrotum is a loose sac of skin that hangs outside the pelvic cavity between the upper thighs. It is divided into two compartments, each holding a testis. The scrotum holds the testes away from the body since normal body temperature is too warm for sperm to be produced. The temperature inside the scrotum is a few degrees cooler than inside the rest of the body. If the external temperature becomes very cold, muscles in the scrotum pull the testes closer to the body, maintaining the proper temperature for sperm production.
The penis is a tubular organ that surrounds the latter part of the urethra. It serves two purposes: to conduct urine outside the body and to deliver semen into the female reproductive tract. The two main parts of the penis are the glans (enlarged tip) and shaft (body). A fold of skin called the prepuce or foreskin covers the glans. It is common practice in certain cultures and religions to remove the foreskin surgically soon after birth, a procedure called a circumcision. The shaft contains three masses or columns of erectile tissue. Normally, this spongy tissue is not filled with much blood. During sexual arousal, however, blood flow to the tissue increases. The penis, engorged with blood, becomes longer, wider, and rigid. This event, called an erection, allows the penis to enter the female vagina and deliver semen to the female's reproductive tract.
The female reproductive system
The reproductive system in females is more complex than that in males. The system produces female gametes, called ova or eggs, and provides a protective space for an ovum to be fertilized and to develop until birth. The primary organs in this system are the ovaries. The accessory organs include the fallopian tubes, the uterus, the vagina, the genitalia, and the mammary glands.
THE OVARIES. The ovaries are two almond-shaped structures measuring about 1.5 inches (3.8 centimeters) in length. They are located on each side of the pelvis, one at the end of each fallopian tube. Ligaments attach the
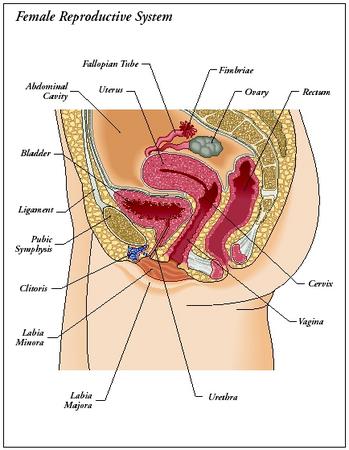
ovaries to the walls of the pelvis and to the uterus (these latter ligaments are called ovarian ligaments).
Within each ovary are many tiny saclike structures called ovarian follicles. An ovary contains several hundred thousand of these follicles, which are present from birth. Each follicle consists of an immature or developing egg called an oocyte surrounded by one or more layers of cells called follicle cells. During a woman's life, however, only about 360 to 480 ovarian follicles will produce mature eggs or ova.
FALLOPIAN TUBES. The fallopian tubes, also called uterine tubes, connect the ovaries to the uterus. Each fallopian tube is about 4 inches (10 centimeters) in length and extremely narrow. The end of the tube that attaches
to an ovary has fingerlike projections called fimbriae that partially surround the ovary. The inner surfaces of the tubes are carpeted with cilia, microscopic hairlike structures projecting in from the inner lining.
THE UTERUS. The uterus, or womb, is a hollow, muscular chamber shaped like an upside-down pear. An average uterus measures about 3 inches (7.6 centimeters) in length and 2 inches (5 centimeters) in width. It weighs approximately between 1 and 1.4 ounces (30 and 40 grams). The uterus lies in the pelvis between the urinary bladder and rectum and is anchored in place by various ligaments.
The part of the uterus above where the fallopian tubes attach is called the fundus. The body is the large central portion. The narrow, lower end that projects a short distance and opens into the vagina is called the cervix.
The thick wall of the uterus is composed of two main layers: the myometrium and the endometrium. The myometrium, the outer layer, is made of smooth muscle cells (among the strongest in the body) that are interwoven to allow the uterus to expand to accommodate a growing fetus and to contract to force the fetus out at the end of pregnancy. The endometrium, the inner layer, provides a site for a fertilized egg to attach to receive nourishment during its development. If an egg is not fertilized, the endometrium sloughs off or is shed during the regular menstrual cycle.
THE VAGINA. The vagina is a muscular tube extending from the uterus to the genitalia. It lies parallel to the rectum. The vagina serves as a exit for menstrual fluids, receives the penis during intercourse, and forms the birth canal through which the fetus passes at the end of pregnancy. Normally, it measures about 4 inches (10 centimeters) in length, but to accommodate all of its activities, its length and width vary widely.
The external opening of the vagina (vaginal opening) is usually partially covered by a thin membrane called the hymen. This membrane is usually ruptured or broken during a women's first sexual intercourse, by the use of tampons during the menstrual period, or during a sports activity.
Bacteria normally exist in the vagina, living on nutrients found in the mucus secreted by the cervix. They are quite beneficial. Through their activities, they create an acidic environment in the vagina that inhibits or prevents the growth of pathogens (disease-causing organisms).
FEMALE GENITALIA. In females, the external sex organs are collectively called the vulva. The parts making up the vulva include the mons pubis, labia majora and minora, clitoris, and greater vestibular glands.
The mons pubis is the prominent fatty bulge at the top of the vulva. Beginning at puberty, this area is covered with pubic hair. Running down from the mons pubis are two hair-covered skin folds or flaps called the labia majora. They enclose two delicate, hair-free skin folds called the labia minora. The area within the labia minora, referred to as the vestibule, contains the openings of the urethra (through which urine passes) and the vagina.
At the top of the labia minora (above the urethral opening) lies the clitoris. A small protruding mass of erectile tissue, it is similar to the male penis. During sexual arousal or excitement, the sensitive clitoris becomes engorged with blood. Located in the floor of the vestibule on either side of the vaginal opening are a pair of glands called the greater vestibular glands. During sexual arousal, these glands secrete a mucus that lubricates the lower portion of the vagina.
MAMMARY GLANDS. Mammary glands are found in the breasts of both women and men. However, they normally function only in women. Mammary glands are modified sweat glands that are actually part of the integumentary system (skin). Although not directly involved in the reproduction process, mammary glands play an important role in providing nourishment for a newborn baby and their activities are controlled by hormones of the reproductive system. For these reasons, they are considered accessory reproductive organs.
On the outside of each breast, slightly below center, is a darkened, reddish brown area called the areola. In the center of the areola is a small protruding nipple.
Within each mammary gland are 15 to 25 lobes radiating inward from the nipple. The lobes are separated by connective tissue and fat. Within each lobe are chambers containing alveolar glands, which produce milk after a woman has given birth. Lactiferous ducts carry milk from the alveolar glands to small openings on the surface of each nipple. The milk is a mixture of water, proteins, fats, sugars, salts, and enzymes that have immune properties.
When a baby suckles a mother's nipple, nerve impulses are sent to the mother's hypothalamus. It then signals the posterior portion of the pituitary gland to secrete the hormone oxytocin. The hormone stimulates the contraction of the muscle cells around the lactiferous ducts, causing the ejection of milk through the nipple.

Comment about this article, ask questions, or add new information about this topic: