Muscle Diseases - Infections of the nervous system
Like any other organ system, the brain and its associated structures may be host to infection. These infections are usually serious because of the significantly high death rate and incidence of residual defects. If the brain is involved in the inflammation, it is known as encephalitis; inflammation of the brain coverings, or meninges , is called meningitis .
Encephalitis
Encephalitis is usually caused by a virus and, because the symptoms are not specific, the diagnosis is usually made by special viral immunologic tests. Both sexes and all age groups can be afflicted. Most patients complain of fever, headache, nausea or vomiting, and a general feeling of malaise. The mental state varies from one of mild irritability to lethargy or coma, and some patients may have convulsions. The physician may suspect encephalitis after completing the history and the physical examination, but the diagnosis is usually established by laboratory tests that include examination of the cerebrospinal fluid (CSF), the EEG, and viral studies of the blood, CSF, and stool. Because there is no specific treatment for viral encephalitis at the present time, particular attention is paid to general supportive care.
Meningitis
Meningitis can occur in either sex at any time of life. The patient often has a preceding mild respiratory infection and later complains of headache, nausea, and vomiting. Fever and neck stiffness are usually present early in the course of the disease, at which time the patient is commonly brought to the physician for examination. If there is any question of meningitis, a lumbar puncture is performed and the CSF examined. It is not possible to make a specific diagnosis of meningitis without examination of the cerebrospinal fluid.
Meningitis is usually caused by bacteria or a virus. It is important to learn what the infectious agent is in order to begin appropriate therapy. Bacterial infections can be treated by antibiotics, but there is no known specific treatment for viral ( aseptic ) meningitis. Meningitis is a life-threatening disease and, despite modern antibiotic therapy, the mortality rate varies from 10 to 20 percent.
Poliomyelitis
Poliomyelitis is an acute viral illness affecting males and females at any time of life, though most commonly before the age of ten. It is also called polio , infantile paralysis , or Heine-Medin disease .
Polio is caused by a virus that probably moves from the gastrointestinal tract via nerve trunks to the central nervous system, where it may affect any part of the nervous system. The disease, however, most often involves the larger motor neurons ( anterior horn cells ) in the brain stem and spinal cord, with subsequent loss of nerve supply to the muscle. The neuron may be partially or completely damaged; clinical recovery is, therefore, dependent on whether those partially damaged nerves can regain normal function.
There are two categories of polio victims: asymptomatic and symptomatic. Those persons who have had no observed symptoms of the disease, but in whom antibodies to polio can be demonstrated, belong in the asymptomatic group. The symptomatic group, on the other hand, comprises patients who have the clinical disease, either with residual paralysis (paralytic polio) or without paralysis (nonparalytic polio).
Symptoms
The symptoms of poliomyelitis are similar to those of other acute infectious processes. The patient may complain of headache, fever, or coryza (head cold or runny nose), or he may have loose stools and malaise. One-fourth to one-third of patients improve for several days only to have a recurrence of fever with neck stiffness. Most patients, however, do not improve, but rather have a progression of their symptoms, marked by neck stiffness and aching muscles. They are often irritable and apprehensive, and some are rather lethargic.
Whether or not the patient will have muscle paralysis should be evident in the first few weeks. Some have muscle paralysis with the onset of symptoms; others become aware of loss of muscle function several weeks after the onset. About half of the patients first notice paralysis during the second to the fifth day of the disease. Patients experience a muscle spasm or stiffness, and may complain of muscle pain, particularly if the muscle is stretched.
The extent of the muscle paralysis is variable, ranging from mild localized weakness to inability to move most of the skeletal muscles. Proximal muscles (those close to the trunk, like the shoulder-arm or hip-thigh) are involved more often than distal muscles (of the extremeties), and the legs are affected more often than the arms. When the neurons of the lower brain stem and the spinal cord at the thoracic level and above are affected, the patient may have a paralysis of the muscles used in swallowing and breathing. This circumstance, obviously, is life-threatening, and particular attention must be paid to the patient's ability to handle saliva and to breathe. If independent, spontaneous respiration is not possible, patients must be given respiratory assistance with mechanical respirators.
Treatment
There is no specific treatment for acute poliomyelitis. The patient should be kept at complete bed rest and given general supportive care, assuring adequate nutrition and fluid intake. Muscle spasm has been treated with hot as well as cold compresses, and no one method has been universally beneficial. Careful positioning of the patient with the musculature supported in a position midway between relaxation and contraction is probably of benefit, and skilled physical therapy is of great importance.
Immunization
Since the early 1900s, attempts had been made to produce an effective vaccine against poliomyelitis, with success crowning the efforts of Dr. Jonas Salk in 1953. Today, vaccination is accomplished with either the Salk vaccine (killed virus), which is given intramuscularly, or the Sabin (live attenuated virus), given orally. There is little question that immunization with poliomyelitis vaccine has proven to be highly effective in eradicating the clinical disease within the community, and it is now a part of routine immunization for all children.
Dementia
Dementia is a term for mental deterioration, with particular regard to memory and thought processes. Such deterioration can be brought about in various ways: infection, brain injury, such toxic states as alcoholism, brain tumors, cerebral arteriosclerosis, and so forth.
The presenile dementias ( Alzheimer's disease ) represent a group of degenerative diseases of the brain in which mental deterioration first becomes apparent in middle age. Commonly, the first clue may be demonstrations of unusual unreasonableness and impairment of judgment. The patient can no longer grasp the content of a situation at hand and reacts inappropriately. Memory gradually fades and recent events are no longer remembered, but events that occurred early in life can be recalled. The patient may wander aimlessly or get lost in his own house. There is progressive deterioration of physical appearance and personal hygiene, and, finally, the command of language deteriorates. Unfortunately, there is a relentless progression of the process, and the patient becomes confined to bed and quite helpless.
Whether the mental deterioration seen in some aged patients, senile dementia, is a specific brain degeneration or is secondary to cerebral arteriosclerosis is not yet settled. It does appear, however, that senile dementia is probably secondary to a degenerative process similar to that of Alzheimer's disease but occurring late in life.
Whether or not dementia can be halted depends upon its cause. If, for example, the dementia is secondary to brain infection or exposure to toxic material, eradication of the infectious agent or removal of the toxin may be of distinct benefit in arresting the dementing process. Unfortunately, there is no specific treatment for the brain degenerative processes.
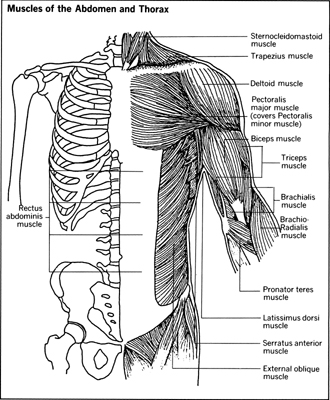
Muscle Diseases
W hen one hears the words “muscle disease,” one may think of only muscular dystrophy and picture a small child confined to a wheelchair. But there are many diseases other than muscular dystrophy in which muscle is either primarily or secondarily involved, and many of these diseases do not have a particularly bad prognosis. Muscle diseases may make their presence known at any time, from early infancy to old age; no age group or sex is exempt.
Any disease of muscle is called a myopathy . The hallmark of muscle disease is weakness, or loss of muscle power. This may be recognized in the infant who seems unusually limp or hypotonic . Often the first clue to the presence of muscle weakness is a child's failure to achieve the developmental milestones within a normal range of time. He may be unusually clumsy or have difficulty in running, climbing stairs, or even walking. Occasionally a teacher is the first one to be aware that the child cannot keep up with classmates and reports this fact to the parents. The onset of the muscle weakness can be so insidious that it may go unnoticed or be misinterpreted as laziness until there is an obvious and striking loss of muscle power.
This is true in the adult as well who at first may feel tired or worn out and then realize that he cannot keep up his previous pace. Often his feet and legs are involved in the beginning. He may wear out the toes of his shoes and may then recognize that he must flex his ankles more to avoid tripping or dragging the toes. Or he finds that he must make a conscious effort to raise the legs in climbing stairs; he may even have to climb one step at a time. Getting out of bed in the morning may be a chore, and rising from a seated position in a low chair or from the floor may be difficult or impossible. Those with arm involvement may recognize that the hands are weak; if the shoulder muscles are involved, there is often difficulty in raising the arms over the head. The patient may take a long time in recognizing the loss of muscle power because the human body can so well compensate or use other muscles to perform the same motor tasks. If the weakness is present for a considerable length of time, there may be a wasting, or a loss of muscle bulk.
Diagnostic Evaluation of Muscle Disease
In evaluating patients with motor weakness, the physician must have a complete history of the present complaints, past history of the patient, and details of the family history. A general physical and neurological examination is required, with particular reference to the motor, or musculoskeletal system. In most cases, the physician will be able to make a clinical diagnosis of the disease process, but occasionally the examination does not reveal whether the nerve, the muscle, or both are involved. In order to clarify the diagnosis, some additional examinations may be required, mainly determination of serum enzymes (a good indicator of loss of muscle substance), a muscle biopsy, and an electromyogram.
Serum Enzymes
Enzymes are essential for the maintenance of normal body chemistry. Because the normal concentration in the blood serum of some enzymes specifically related to muscle chemistry is known, the determination of concentrations of these enzymes can provide additional evidence that muscle chemistry is either normal or abnormal.
Muscle Biopsy
The first step is the surgical removal of a small segment of muscle, which is then prepared for examination under the microscope. The examination enables the physician to see any abnormality in the muscle fibers, supporting tissue, small nerve twigs, and blood vessels. The muscle biopsy can be of great value in making a correct diagnosis, but occasionally, even in good hands, there is not sufficient visible change from the normal state to identify the disease process.
Electromyograph (EMG)
This is a technique for studying electrical activity of muscle. Fine needles attached to electronic equipment are inserted into the muscle to measure the electrical activity, which is displayed on an oscilloscope , a device something like a television screen. It is not a particularly painful process when performed by a skilled physician, and the information gained may be important in establishing a diagnosis.

Comment about this article, ask questions, or add new information about this topic: