Diseases of the Blood - Red cell diseases
Half the blood is plasma; the other half is made up of many tiny blood cells. The biggest group in number is the red blood cells. These cells contain a complicated chemical called hemoglobin , which brings oxygen from the lungs to body cells and picks up waste carbon dioxide for expiration. Hemoglobin is rich in iron, which is what imparts the characteristic red color to blood.
Red blood cells are manufactured by bones all over the body—in the sternum, ribs, skull, arms, spine and pelvis. The actual factory is the red bone marrow, located at bone ends. As red cells mature and are ready to enter the bloodstream, they lose their nuclei to become what are called red corpuscles or erythrocytes . With no nucleus, a red corpuscle is relatively short-lived (120 days). Thus, the red cell supply must be constantly replenished by bone marrow. And a busy factory it is because 20 to 25 trillion red corpuscles normally travel in the circulation. The spleen is responsible for ridding the body of the aged corpuscles, but it is not an indiscriminate sanitizer; it salvages the hemoglobin for reuse by the body.
To measure levels of red cells, physicians make a blood count by taking a smidgen of blood from a patient's fingertip. The average number of red cells in healthy blood is about five million per cubic millimeter for men, and four and one-half million for women.
Anemia
Anemia exists when the red cell count stays persistently below four million. Abnormalities in the size, shape, or hemoglobin content of the erythrocytes may also account for anemic states. Any such irregularity interferes with the red cell's ability to carry its full share of oxygen to body tissues. It also tends to weaken the red cells so that they are more likely to be destroyed under the stresses of the circulation.
Anemia may result from:
- • nutritional deficiencies that deprive the body of elements vital to the production of healthy cells
- • diseases or injuries to organs associated with either blood cell formation (bone marrow) or blood cell destruction (spleen and liver)
- • excessive loss of blood, the consequences of surgery, hemorrhage, or a bleeding ulcer and
- • Heredity, as in the case of sickle cell anemia (where the red cells are misshapen)
Hemolytic Anemia
There are also several kinds of disorders known as hemolytic anemias that are linked to the direct destruction of red cells. Poisons such as snake venom, arsenic, and lead can cause hemolytic anemia. So can toxins produced by certain bacteria as well as by other organisms, such as the parasites that cause malaria, hookworm, and tapeworm. Destruction of red cells may also stem from allergic reactions to certain drugs or transfusions with incompatible blood.
The various anemias range from ailments mild enough to go undetected to disorders that prove inevitably fatal. Many are rare; following are the more common.
Pernicious Anemia
Pernicious anemia, or Addison's anemia , is associated with a lack of hydrochloric acid in the gastric juices, a defect which interferes with the body's ability to absorb vitamin B 12 from the intestine. Because the vitamin acts as an essential stimulus to the production of mature red blood cells by the bone marrow, its lack leads to a reduced output. Moreover, the cells tend to be larger than normal, with only half the lifespan of the normal erythrocyte.
The symptoms are characteristic of most anemias: pale complexion, numbness or a feeling of “pins and needles” in the arms and legs, shortness of breath (from a lack of oxygen), loss of appetite, nausea, and diarrhea (often accompanied by significant weight loss). One specific feature is a sore mouth with a smooth, glazed tongue. Advanced stages of the disease may be marked by an unsteady gait and other nervous disorders, owing to degeneration of the spinal cord. Red cell count may drop to as low as 1,000,000. Several kinds of tests may be necessary to differentiate pernicious anemia from other blood diseases—a test for hydrochloric acid levels, for example.
Pernicious anemia, however, is no longer so pernicious, or deadly, as it once was—not since its cause was identified. Large, injected doses of vitamin B;i1;i2 usually restore normal blood cell production.
Sickle Cell Anemia
Sickle cell anemia, an inherited abnormality, occurs almost exclusively among black people. Widespread in tropical Africa and Asia, sickle cell anemia is also found in this country, affecting perhaps 1 in 500 American blacks. The red blood cells are sickle-shaped rather than round, a structural aberration arising from a defect in the manufacture of hemoglobin, the oxygen-carrying component. Such mis-shapen cells tend to clog small blood vessels, depriving organs and tissues of oxygen. Sickle cells live only 10 to 20 days, as compared to 120 for normal red blood cells. They cannot be replaced fast enough, causing anemia.
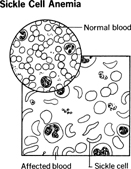
A differentiation should be made between sickle cell anemia, the full-blown disease, and sickle cell trait. Anemia occurs when the offspring inherits the sickle cell gene from both parents. In some patients the symptoms are mild; in others, they are severe. The disease can cause pain and swelling in the feet and hands, along with fever; fatigue, paleness, and shortness of breath; severe pain that can last from hours to weeks, sometimes requiring hospitalization; retinal damage that can be serious enough to cause blindness; jaundice; delayed growth and puberty in children and slightness of build in adults; infections; susceptibility to strokes in children; and acute chest syndrome, a life-threatening condition caused by infection or trapped sickle cells in the lung. Sickle cell anemia is a very serious disease for which there is no cure, but there are treatments that can help, including painkilling drugs, penicillin, and blood transfusions. The anticancer drug hydroxyurea reduces the frequency of painful episodes and of acute chest syndrome and lessens the need for transfusions.
Sickle cell anemia was once fatal to most of its victims by the age of 30. Today, with good medical care, many people with sickle cell anemia can live into their 40s and even beyond.
Those with only one gene for the disease have sickle cell trait . They are not likely to have too much trouble except in circumstances where they are exposed to low oxygen levels (the result, say, of poor oxygenation in a high-altitude plane). Administration of anesthesia or too much physical activity may also bring on some feverish attacks. Those with the trait can pass it on to the next generation. One in 12 black Americans carries the trait.
Iron-Deficiency Anemia
Iron-deficiency anemia is a common complication of pregnancy, during which time the fetus may rob the maternal blood of much of its iron content. Iron is essential to the formation of hemoglobin. The deficiency can be further aggravated by digestive disturbances (e.g., a lack of hydrochloric acid) that may hinder the absorption of dietary iron from the intestines. Some women may not observe proper dietary habits, thereby aggravating the anemic state. Successful treatment involves increasing iron intake, with iron supplements and an emphasis on iron-rich foods, including eggs, cereals, green vegetables, and meat, especially liver.
Polycythemia
Polycythemia is the opposite of anemia; the blood has too many red corpuscles. The most common form of the disease is polycythemia vera (or erythremia ). In addition to the rise in corpuscle count, there is a corresponding rise—as much as threefold—in blood volume to accommodate the high cell count, and increased blood viscosity. Symptoms include enlarged spleen, bloodshot eyes, red mouth, and red mucous membranes—all resulting from excess red cells. Other common characteristics are weakness, fatigue, irritability, dizziness, swelling in the ankles, choking sensations, vise-like chest pains (angina pectoris), rapid heartbeat, and sometimes severe headaches. There is also an increased tendency toward both clotting and hemorrhaging.
The disease occurs primarily in the middle and late years and is twice as prevalent in males as in females. The cause is unknown, but polycythemia is characterized by stepped-up bone marrow production activity.
Radioactive phosphorus therapy is one method for controlling this hyperactivity. Low iron diets and several forms of drug therapy have been tried with varying degrees of effectiveness. A one-time panacea, bloodletting—to drain off excess blood—appears to be of considerable value. Many patients survive for years with the disease. Premature death is usually the result of vascular thrombosis (clotting), massive hemorrhage, or leukemia.
The Rh Factor
Rh disease might also be considered a form of anemia—in newborns. The disorder involves destruction of the red blood cells of an as-yet unborn or newborn infant. It is brought about by an incompatibility between the maternal blood and fetal blood of one specific factor—the so-called Rh factor. (Rh stands for rhesus monkey, the species in which it was first identified.) Most of us are Rh positive, which is to say that we have the Rh protein substance on the surface of our red cells. The Rh factor is, in fact, present in 83 percent of the white population and 93 percent of the black. Those lacking it are classified as Rh negative.
A potentially dangerous situation exists when an Rh negative mother is carrying an Rh positive baby in her uterus. Although the mother and unborn baby have separate circulatory systems, some leakage does occur.
When Rh positive cells from the fetus leak across the placenta into the mother's blood, her system recognizes them as foreign and makes antibodies against them. If these antibodies then slip across into the fetal circulation, damage is inevitable.
The first baby, however, is rarely affected because it takes time for the mother's body to become sensitized to the Rh positive cells. But should she become pregnant with another child, the now-sensitized mother's blood produces a large quantity of destructive antibodies that could result in stillbirth, death of the infant shortly after birth or, if the child survives, jaundice and anemia.
Modern medicine has reduced the fatality rate and considerably improved the prognosis. Severely affected newborns are being treated by complete blood transfusion—even while still in the womb—to draw off all the Rh positive cells. After birth and as it grows older, the child will once again produce Rh positive cells in its bone marrow—but by that time the danger from the mother's antibodies is past. Recently an Rh vaccine to prevent the problem from ever occurring was developed. After Rh negative women give birth to their first Rh positive baby, they are immunized with the anti-Rh serum to prevent them from manufacturing these dangerous antibodies.

Comment about this article, ask questions, or add new information about this topic: